Shoulder impingement is an overuse injury that causes achy pain on the front or side of the shoulder. The pain is felt most when the arm is overhead or extended to the side. Shoulder impingement also is called rotator cuff tendonitis, subacromial impingement, supraspinatus tendonitis, and shoulder bursitis.
Shoulder impingement is common in swimmers and athletes who play baseball, tennis, and volleyball. It can also occur in weight lifters, gymnasts, divers, and rowers. Causes include a rapid increase in overhead activity, weakness or strength imbalance in the rotator cuff or scapular muscles, postural abnormalities, shoulder joint instability, or improper training or technique.
The following is information from the American Academy of Pediatrics summarizing treatment phases and goals for shoulder impingement.
Phases and Goals of Shoulder Impingement Treatment
Treating shoulder impingement involves limiting activities that cause pain and using ice and nonsteroidal anti-inflammatory drugs (NSAIDs) to help reduce inflammation. The symptoms of shoulder impingement will subside with rest, but the condition will not fully resolve until the underlying causes have been identified and corrected.
| I |
Pain control |
- Limit overhead activity or anything that causes pain.
- Pitchers- Limit pitching; may try playing first or second base.
- Tennis- Limit serves and overhead shots.
- Swimmers- Limit butterfly, freestyle, and hand paddles.
- Ice, NSAIDs.
|
- The other phases of rehabilitation will not be effective until pain is controlled.
- Swelling inside the shoulder may worsen the pain and contribute to further injury.
- Pain may be reduced by limiting other activities or changing technique for painful activities.
|
| II |
Therapeutic exercise
Correct poor posture. Restore strength to scapular stabilizers. |
- Stretch anterior chest wall muscles; strengthen inter-scapular muslces with rowing-type exercises (Figure 1), and strengthen scapular stabilizers with shoulder protraction exercises (Figure 2).
- Use elastic tubing or weights to strengthen external rotators of shoulder.
|
Proper posture is very important- chest out and shoulders back. These exercises strengthen parts of the body that help with posture and holding the shoulder bones in the proper position. |
| III |
Maintain fitness; strengthen related areas |
- Continue with aspects of the sport that don't require overhead motion or cause pain.
- General conditioning, including aerobic exercise (running, cycling, kicking drills for swimmers).
- Lower extremity and trunk strengthening.
|
Strength in the legs, hips, and trunk is crucial for maximizing arm strength and power with throwing or tennis. This part of rehabilitation can usually take place while shoulder pain is subsiding. |
| IV |
Restore function |
- Resume overhead motion gradually as symptoms permit.
- Correct technique or training.
|
- For pitchers, follow a graded return-to-throwing program.
- Consider biomechanical assessment if technique errors are suspected in a pitcher, swimmer, or tennis player.
|
| V |
Maintenance therapy; prevent recurrent injury |
Continue with maintenance exercises that have been prescribed and any corrections in technique or training regimens that helped with recovery. Include exercises that help prevent the strength imbalances that occur with repetitive overhead activity and contribute to injury. |
Athletes should continue select important exercises after therapy. These are typically not as extensive or time-consuming as the rehabilitation program. |
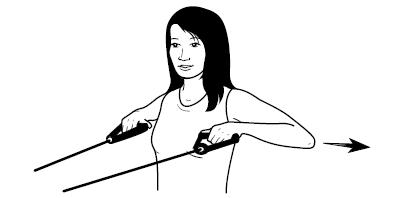
Figure 1. Strengthening inter-scapular muscles with elastic tubing.
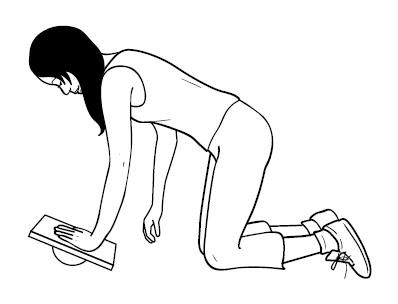
Figure 2. Shoulder protraction exercise (balance with one arm on wobble board or deflated ball).