By: Yvonne A. Maldonado, MD, FAAP
Polio is caused by a virus that affects infants and young children more often than other age groups. Most cases of polio are mild. Rarely, polio infection also can be much more severe and can cause paralysis. Paralytic polio causes muscles to be paralyzed—leaving some people physically impaired for the rest of their lives.
(See "I'm a Polio Survivor. I Don't Want You to Get It" below.)
Polio: a vaccine success story
Before the polio vaccine, widespread cases of paralytic polio in the U.S. led many parents to be worried about letting their children swim in public swimming pools or get together at neighborhood movie theaters.
Since the mid-1950s, the polio vaccines have led to a dramatic decline—with over a 99% reduction in polio cases around the world. The "natural" or "wild" type of poliovirus that infected children decades ago is eliminated from the U.S. and much of the rest of the world.
The polio vaccine is recommended for children by the
American Academy of Pediatrics. If you think your child has fallen behind on immunizations, talk with your pediatrician.
I'm A Polio Survivor. I Don't Want You to Get It.
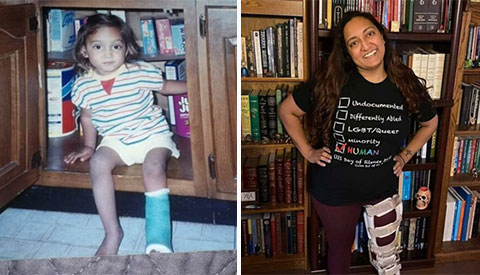 In July 2022, an unvaccinated 20-year-old in
New York, was diagnosed with paralytic polio, a disease that's almost wiped out. Many ask, "How did this happen?" To polio survivors like me, it was only a matter of "when," not "how."
In July 2022, an unvaccinated 20-year-old in
New York, was diagnosed with paralytic polio, a disease that's almost wiped out. Many ask, "How did this happen?" To polio survivors like me, it was only a matter of "when," not "how."
In 2020, thousands of people, including politicians, health "experts" and the general public shared
harmful myths about COVID vaccines. These people do not think of the dangers that their actions pose to the long-term health of themselves and their community.
They forget people like me and others who survived past vaccine-preventable diseases.
I contracted polio in 1992 in India when I was less than a year old. Shortly after, I was adopted and raised in Saint Louis by a phenomenal and supportive family. Despite my family's great insurance and access to world-class medical care, polio is not an easy ride.
One in 200 polio infections are paralytic—mine was one of them.
Surprisingly, paralysis and a leg brace are the least annoying side effects. The long-term neurological consequences of
post-polio syndrome are arguably worse. Post-polio is the further weakening of muscles that may or may not have been affected during the initial polio infection. It occurs 15 to 40 years later in 25% to 40% of polio survivors. If someone has paralytic polio, they are more likely to be affected with post-polio.
What are the silent side effects of a disease long forgotten? Personally, the constant cold feeling is truly the worst. Poliovirus
affects the hypothalamus, which makes it hard to regulate body temperature. Ask any polio survivor and we will tell you that we are always cold; our feet are bluish-purple. We perceive the air temperature to be about 20 degrees cooler. A 70-degree room will feel like 50 degrees. You can always find me with a jacket on or under three blankets.
Chronic fatigue is another hurdle in our lives. I describe polio as living at 20% battery and being easily overexerted. Muscles that are not affected by polio are strained, causing our bodies to become even more exhausted.
People may not realize that polio affects every body system, not just lungs or a paralyzed leg. Families do not realize the day-to-day reality of disability or the logistics and planning involved to keep functioning in a world not made for disabilities.
With the goal of preventing another child from getting sick, I began my advocacy work in 2005 with Shriners Hospital. Since then, I have spoken to groups such as Rotary, the Saint Louis Cardinals, NFL and college football teams, and (my personal favorite speaking gig) a Trans-Siberian Orchestra concert! Yet myths about routine vaccines now threaten the progress we've made throughout my lifetime.
False ideas are why a 20-year-old was diagnosed with polio in 2022. Harmful ideas are why hundreds of thousands of people unnecessarily died of COVID instead of being vaccinated. And as long as made-up myths go unchecked, vaccine-preventable diseases like polio will remain prevalent and history may repeat itself.
Grace R. is a polio survivor and vaccine advocate from Illinois. Her story originally appeared on the Voices for Vaccines blog.
How does polio spread?
Polio can spread to other people through contact with stool (poop) from an infected person or droplets from a sneeze or cough. It is transmitted from contact with fecal matter (stool or poop) within one to two weeks after a person is infected with polio. A person who gets stool or droplets from an infected person on their hands will get infected if they touch their mouth. Children who are not vaccinated can get infected if they put toys or other objects that have stool or droplets on them into their mouth.
An infected person can spread poliovirus to others before they have symptoms. The virus can live in an infected person's stool for weeks. People can contaminate food and water if they touch it with unwashed hands.
It is hard to detect polio or prevent it from spreading. Anyone who is not immunized is at risk.
What are the symptoms of polio?
Most people with polio infection will have no symptoms. Infrequently, polio can cause paralysis in the arms and legs or death if muscles involved in breathing are paralyzed.
Symptoms may begin with a low-grade fever and a sore throat about 6 to 20 days after being exposed to the virus. Children also may feel pain or stiffness in their back, neck and legs for a brief time. Paralysis causes severe muscle pain.
A person is most contagious 7 to 10 days before symptoms occur and can infect others for another 7 to 10 days.
Is there a cure for polio?
No treatment is available for polio. Some children fully recover from polio, but others are disabled for a lifetime or may die from the disease.
The best protection is the polio vaccine. In the United States, the inactivated polio vaccine (IPV) is the only vaccine recommended. IPV is given as a shot (injection) by trained health workers.
Children should get four doses of IPV when they are 2 months old, 4 months old, between age 6 months and age 18 months, and between age 4 years and age 6 years. If your family is planning to
travel to a country that has a high risk of polio, talk to your pediatrician before your trip.
Why the inactivated polio vaccine is recommended
Some countries continue to provide live, oral polio virus vaccines (OPV), which have not been given in the United States since 1999. The OPV is not a shot. It is given by mouth. Anyone given the OPV who is exposed to polio viruses can still be infected. If they are vaccinated, they are protected from developing symptoms including paralysis. However, they can still spread the virus to others, including those who are not vaccinated. That is why it is important for all children to continue to receive polio vaccines.
Polio reported in the United States
A case of paralytic polio from an
oral polio virus vaccine (OPV) was reported in an unvaccinated adult in New York in July 2022. This was the first case in the United States in almost 10 years.
Most people in the United States have been vaccinated against polio and are at very low risk for polio infection and paralysis. People who have not been vaccinated or who have not received all doses of polio vaccine are at higher risk if they are exposed to someone who is infected with polio or someone who received the oral polio vaccine.
More information
About Dr. Maldonado
 Yvonne (Bonnie) Maldonado, MD, FAAP, is Senior Associate Dean for Faculty Development and Diversity and the Taube Endowed Professor of Global Health and Infectious Diseases; Professor of Pediatrics and of Epidemiology and Population Health; Chief of the Division of Pediatric Infectious Diseases at Stanford University School of Medicine and Medical Director of Infection Prevention and Control and Attending Physician at Lucile Packard Children's Hospital at Stanford University.
Yvonne (Bonnie) Maldonado, MD, FAAP, is Senior Associate Dean for Faculty Development and Diversity and the Taube Endowed Professor of Global Health and Infectious Diseases; Professor of Pediatrics and of Epidemiology and Population Health; Chief of the Division of Pediatric Infectious Diseases at Stanford University School of Medicine and Medical Director of Infection Prevention and Control and Attending Physician at Lucile Packard Children's Hospital at Stanford University.
|