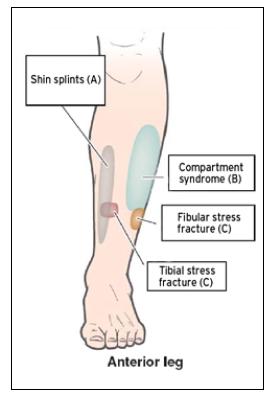
Shin pain occurs most frequently in athletes involved in running, jumping, or high-impact sports. Shin pain can be caused by shin splints (also called medial tibial stress syndrome), a stress fracture of the tibia or fibula, or compartment syndrome. The most common source of shin pain in runners is shin splints.
Symptoms
For all of the different causes of shin pain, athletes often complain first of pain, burning, or tightness along the shin. The following are symptoms of bone-related and musclerelated shin pain.
Symptoms of bone-related shin pain may include:
- Pain in a very focal area of the shin
- Pain during and after running
- Pain that gets worse over time
Symptoms of muscle-related shin pain may include:
- Mild soreness
- Tightness or pressure in shins with running
- Pain only with running, relieved by rest
- No pain when pushing on the bone
- Numbness, tingling, or weakness in the foot
Causes
Shin pain is generally the result of one or more of the following issues:
- Body mechanics refers to the way the body moves while in motion. Athletes may experience pain due to poor body mechanics. The way the body moves can be influenced by different factors. For example, how a runner runs may be affected by foot type, running style, and hip and core (abdominal and back) muscle strength.
- Too much exercise can become a problem if athletes increase too quickly. A helpful reminder is the “10% Rule”: no more than a 10% increase in frequency, duration, or intensity of exercise per week.
- Bone density (bone strength). Softer bones break easier, so if there is a stress fracture that is not explained by poor mechanics or rapid increases in training, bone density might be the problem. The causes of low bone density include
- Genetics (it tends to run in families)
- Not enough calcium in the diet (more than 1,300 mg/day is the recommended daily amount, equal to 3 to 4 servings of milk, yogurt, cheese, or other sources)
- Irregular periods (no menstrual period for more than 6 months in a row), which causes low levels of the hormone estrogen
Tests
Shin splints can be diagnosed by their characteristic symptoms and physical examination findings. A stress fracture is suspected when shin pain becomes more severe, more localized (in a focal area), or if there are risk factors for weaker bones such as the female athlete triad.
X-rays may show a stress fracture if the problem has been present long enough to see a healing response (4–6 weeks). However, x-rays can appear normal even when a stress fracture is known to be present. In order to confirm the presence of a stress fracture, it may be necessary for
magnetic resonance imaging (MRI).
Athletes with compartment syndromes will have normal x-rays and no evidence of bony abnormalities with bone scan or MRI. Compartment syndrome is confirmed by taking a pressure measurement through a needle inserted into the muscle both before and after exercise.
Treatment
A period of rest from running may be needed for the stress fracture or shin splints to heal. Although the athlete may be able to run with shin splints, continuing to do so may cause the shin splints to progress to a stress fracture. During rest, cross-training with nonimpact activities (such as using an elliptical machine,
biking,
swimming, and
weights) can be done if the athlete is pain-free. Ice and
acetaminophen are effective for pain, but nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen may actually slow the healing of some stress fractures. Other treatments like bone stimulators are controversial. In very rare cases rest is not enough for a fracture to heal, and surgery is needed.
Prevention
Shin splints and stress fractures can be reduced by allowing time to gradually build up to higher levels of impact activity (increase by no more than 10% per week). If an athlete has flat feet or high-arched feet, a proper shoe and/or shoe insert may be helpful. Since stress fractures in the shin usually start with shin splints, identifying and treating shin splints—before they progress—can prevent the development of stress fractures. Maintaining healthy bone through good diet (high in
vitamin D and calcium), safe weight loss practices, and attention to any menstrual problems may also reduce the risk of stress fracture.
Compartment syndromes are more difficult to prevent. However, balancing low-impact conditioning with high-impact conditioning, selecting softer surfaces for running, and using a properly cushioned running shoe may help.