By: Christina Boull, MD, FAAD, FAAP
Skin cancer is rare in children. However, following
safe-sun practices is the best way to protect children from developing skin cancer later in life.
For adults, it's a good idea to get regular skin-cancer screenings beginning as early as their 20s. Most children do not need regular skin exams by a dermatologist to monitor for skin cancer unless they have certain risk factors.
As a parent, here's what you should know about skin cancer.
Types of skin cancer
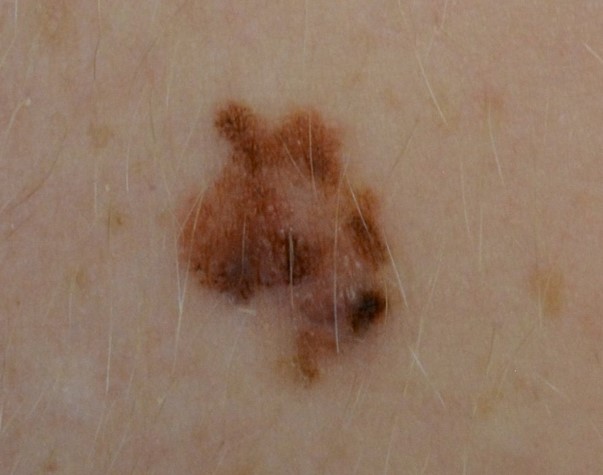 Early detection of melanoma is important, since this type of skin cancer can quickly spread to anywhere in the body. It can even develop on sun-protected skin. Early detection of melanoma is important, since this type of skin cancer can quickly spread to anywhere in the body. It can even develop on sun-protected skin. Melanoma can look like a growing or bleeding pink bump that doesn't go away. It can also look like a brown mole that is changing in shape, color, size, or feel. (See image at right).
|
Non-melanoma skin cancer
Children who are immunosuppressed, meaning their body's defense systems are weakened by certain illnesses, medications, or treatments, are more likely to develop these skin cancers. This may look like a small sore, but will last for more than 8 weeks.
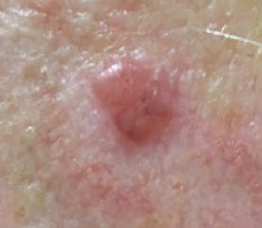
Basal cell carcinoma: Pearly pink bump, scaly spot, or non-healing sore
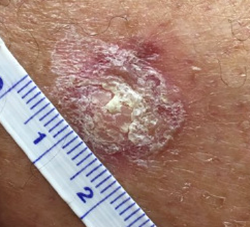
Squamous cell carcinoma: Scaly pink spot, bump, or non-healing sore
|  |
Squamous cell carcinoma
|
Basal cell carcinoma |
Identifying a skin cancer
Skin cancers can appear as pink, growing, or bleeding bumps on previously normal skin. It is normal for children and teens to develop new moles over time. New moles should not continue to grow rapidly or change once they appear. Unexplained bumps that don't go away and non-healing sores that last longer than 8 weeks should be evaluated for skin cancer.
The ABCDE's of concerning moles or spots
These features can be a sign of melanoma
Asymmetry: One side of a mole is different than the other side
Border: Irregular or poorly defined edges
Color: Multiple colors within one mole, pink or red spots instead of brown, or an existing mole that is changing colors
Diameter: Larger than ¼ inch (a pencil eraser) increases risk, but some skin cancers are smaller if found early. This is the least important factor. Some birthmarks (congenital moles) may be larger than this, but do not necessarily have a higher risk of skin cancer.
Evolving: A mole or lesion that looks different from the others, different than it had previously, or is bleeding, itching, or crusting. Moles that are growing rapidly are worrisome. Taking photos can be a helpful way to monitor moles over time.
Risk factors for skin cancer
Hereditary cancer syndromes
Genetic syndromes that increase sun sensitivity
Suppressed immune system: organ or stem cell transplant, chemotherapy or certain medications
History of skin cancer
History of radiation therapy
History of multiple sunburns
Family history of melanoma in a parent or sibling
Medications that make skin easier to damage or burn
Children with these risk factors should talk with their doctor about having a skin exam and consider seeing a dermatologist.
Skin cancer treatment
Many factors are involved with choosing a skin cancer treatment, including type of cancer, size of cancer, and body location. Treatments may include:
Creams that activate the immune system (imiquimod or 5-fluorouracil)
Procedures that scrape, burn, or surgically remove the skin cancer
Oral or intravenous chemotherapy medications
Combination of the above
Your dermatologist will help determine what type of treatment is best for your child's skin cancer.
Preventing skin cancer means preventing sun damage
Luckily, most skin cancers are preventable. Early sun exposure and sunburns are an important risk factor for developing skin cancer. There are many ways to
protect your child from the radiation from the sun:
Seek shade. Avoid outdoor activities during midday hours (10am to 2pm) when the sun is the most intense
Wear a hat with a wide brim that goes all the way around. This protects the scalp, face, ears, and the back of the neck.
Wear long sleeve shirts, full-length pants and sun-protective clothing with ultraviolet protection factor (UPF)*
Wear rash guards (swim shirts) at the pool/beach
Wear sunglasses.
Apply sunscreen with SPF 30 or higher every two hours, more often when swimming or sweating. For children, those containing zinc oxide or titanium dioxide are safe and effective.
Avoid
tanning beds. Rays from tanning beds are even more harmful than those from the sun. Getting a "base tan" is not safe or protective.
More information
About Dr. Boull
 Christina Boull is an Assistant Professor of Pediatrics and Dermatology at the University of Minnesota. She is a board-certified pediatrician and pediatric dermatologist. Her areas of interest include genetic skin diseases and cutaneous malignancies in children. Christina Boull is an Assistant Professor of Pediatrics and Dermatology at the University of Minnesota. She is a board-certified pediatrician and pediatric dermatologist. Her areas of interest include genetic skin diseases and cutaneous malignancies in children.
|
Photos provided by Sheilagh Maguiness, MD, FAAP